Vaccinating for Measles and Mumps (MMR) Outbreaks
Recent outbreaks of mumps have also been reported among adolescents and young adults in the United States and United Kingdom.
The mumps outbreak in the United Kingdom is ongoing.
Recommendations for travelers
All travelers should be fully immunized and keep a copy of their immunization record with them as they travel.
Mumps , Measles & Rubella (MMR) Rubella also called German Measles)
Measles remains a common disease in many parts of the world, including areas in Europe, Asia, the Pacific, and Africa. Worldwide, about 20 million people get measles each year; about 146,000 die.
Most of the measles cases result from international travel. The disease is brought into home countries by unvaccinated people who get infected in other countries. They spread measles to others, which can cause outbreaks.
Anyone who is not protected against measles is at risk of getting infected when they travel internationally.
Make Sure You’re Protected against Measles before International Travel
• Infants 6 months through 11 months of age should receive one dose of MMR vaccine.†
• Children 12 months of age and older should receive two doses of MMR vaccine separated by at least 28 days.
• Teenagers and adults who do not have evidence of immunity* against measles should get two doses of MMR vaccine separated by at least 28 days.
IInfants who get one dose of MMR vaccine before their first birthday should get two more doses (one dose at 12 through 15 months of age and another dose at least 28 days later).
* Acceptable presumptive evidence of immunity against measles includes at least one of the following: written documentation of adequate vaccination, laboratory evidence of immunity, laboratory confirmation of measles, or birth in the United States before 1957.
Get Vaccinated and Prevent Measles talk to Your ITVC Travel Doctor
What are signs and symptoms?
The symptoms of measles generally appear about seven to 14 days after a person is infected.
Measles typically begins with
- high fever,
- cough,
- runny nose (coryza), and
- red, watery eyes (conjunctivitis)).
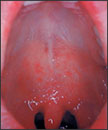
Two or three days after symptoms begin, tiny white spots (Koplik spots) may appear inside the mouth.
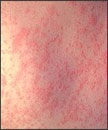
Skin of a patient after 3 days of measles infecti
Mouth of a patient with Koplik spots, an early sign of measles infection.
| Measles Rash | Koplik Spots |
 |
 |
Three to five days after symptoms begin, a rash breaks out. It usually begins as flat red spots that appear on the face at the hairline and spread downward to the neck, trunk, arms, legs, and feet. Small raised bumps may also appear on top of the flat red spots. The spots may become joined together as they spread from the head to the rest of the body. When the rash appears, a person's fever may spike to more than 104° Fahrenheit.
After a few days, the fever subsides and the rash fades.
Mumps
Mumps is viral disease
negative-strand RNA virus called a paramyxovirus
TRANSMISSION
By respiratory droplets, saliva, or contact with contaminated fomites.
Endemic in many countries throughout the world. Mumps vaccine is routinely used in 61% of countries in the world, and the risk of exposure among travelers is high in many countries, including industrialized countries.
CLINICAL Symptoms
Incubation period is 16–18 days (range, 12–25 days). Mumps is characterized by parotitis (swelling of the parotid salivary glands), either unilateral or bilateral. Onset of illness is usually nonspecific, with symptoms of fever, headache, malaise, myalgia, and anorexia. Complications may occur such as orchitis, aseptic meningitis, encephalitis, and pancreatitis. Approximately 20% of cases are asymptomatic
Usually clinical, defined as illness with acute onset of unilateral or bilateral tender, self-limited swelling of the parotid glands, other salivary glands, or both, lasting ≥2 days, and without other apparent cause.
TREATMENT
Supportive care.
PREVENTION
Travelers aged ≥6 months who do not have acceptable evidence of mumps immunity (as documented by 2 doses of live mumps virus vaccine ≥28 days apart on or after the first birthday, laboratory evidence of immunity, laboratory confirmation of disease, or birth before 1957) should be vaccinated with measles-mumps-rubella (MMR) vaccine.
Rubella
The name rubella is derived from Latin, meaning “little red.” Rubella was initially considered to be a variant of measles or scarlet fever and was called “third disease”. It was not until 1814 that it was first described as a separate disease in the German medical literature, hence the common name “German measles”. In 1914,
Rubella virus is classified as a togavirus,
It is most closely related to group A arboviruses,
Pathogenesis
Following respiratory transmission of rubella virus a viremia occurs 5 to 7 days after exposure with spread of the virus throughout the body. Transplacental infection of the fetus occurs during viremia. Fetal damage occurs through destruction of cells as well as mitotic arrest.
Clinical Features
The incubation period of rubella is 14 days, with a range of 12 to 23 days. Symptoms are often mild, and up to 50% of infections may be subclinical or inapparent. In children, rash is usually the first manifestation and a prodrome is rare. In older children and adults, there is often a 1 to 5 day prodrome with low-grade fever, malaise, lymphadenopathy, and upper respiratory symptoms preceding the rash. The rash of rubella is maculopapular and occurs 14 to 17 days after exposure. The rash usually occurs initially on the face and then progresses from head to foot. It lasts about 3 days and is occasionally pruritic. The rash is fainter than measles rash and does not coalesce. The rash is often more prominent after a hot shower or bath. Lymphadenopathy may begin a week before the rash and last several weeks. Postauricular, posterior cervical, and suboccipital nodes are commonly involved.
Arthralgia and arthritis occur so frequently in adults that they are considered by many to be an integral part of the illness rather than a complication. Other symptoms of rubella include conjunctivitis, testalgia, or orchitis.
Complications
Complications of rubella are not common, but they generally occur more often in adults than in children.
Arthralgia or arthritis may occur in up to 70% of adult women who contract rubella, but it is rare in children and adult males. Fingers, wrists, and knees are often affected. Joint symptoms tend to occur about the same time or shortly after appearance of the rash and may last for up to 1 month; chronic arthritis is rare.
Encephalitis occurs in one in 6,000 cases, more frequently in adults (especially in females) than in children. Mortality estimates vary from 0 to 50%.
Hemorrhagic manifestations occur in approximately one per 3,000 cases, occurring more often in children than in adults. These manifestations may be secondary to low platelets and vascular damage, with thrombocytopenic purpura being the most common manifestation. Gastrointestinal, cerebral, or intrarenal hemorrhage may occur. Effects may last from days to months, and most patients recover.
Additional complications include orchitis, neuritis, and a rare late syndrome of progressive panencephalitis.
MMR (Measles, Mumps, and Rubella ) vaccine
Some people should not get MMR vaccine or should wait.
- Anyone who has ever had a life-threatening allergic reaction to the antibiotic neomycin, or any other component of MMR vaccine, should not get the vaccine. Tell your doctor if you have any severe allergies.
- Anyone who had a life-threatening allergic reaction to a previous dose of MMR or MMRV vaccine should not get another dose.
- Some people who are sick at the time the shot is scheduled may be advised to wait until they recover before getting MMR vaccine.
- Pregnant women should not get MMR vaccine. Pregnant women who need the vaccine should wait until after giving birth. Women should avoid getting pregnant for 4 weeks after vaccination with MMR vaccine.
- Tell your doctor if the person getting the vaccine:
- Has HIV/AIDS, or another disease that affects the immune system
- Is being treated with drugs that affect the immune system, such as steroids
- Has any kind of cancer
- Is being treated for cancer with radiation or drugs
- Has ever had a low platelet count (a blood disorder)
- Has gotten another vaccine within the past 4 weeks
- Has recently had a transfusion or received other blood products
- Any of these might be a reason to not get the vaccine, or delay vaccination until later.


